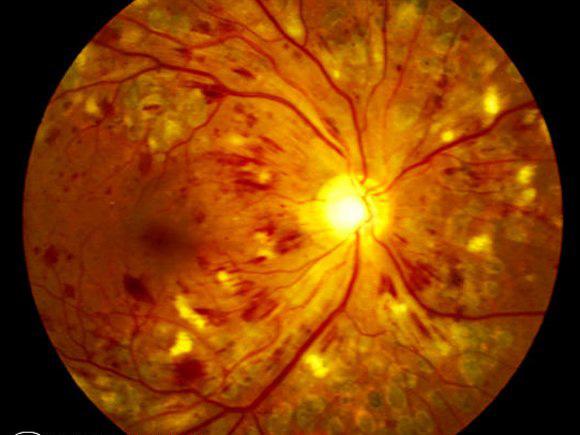
For example, the United Kingdom Prospective Diabetes Study revealed intensive blood sugar control in newly diagnosed patients with Type 2 diabetes had less microvascular complications, including retinopathy, compared with patients who received standard treatment. Multiple clinical studies, as well as epidemiologic studies, support this association. Proliferative diabetic retinopathy is found in approximately 2% of type 2 patients who have diabetes for less than five years, and 25% who have had diabetes for 25 years or more. After 10 years, the numbers increase to 84% and 53%, respectively. 7,8 In Type 2 patients older than age 30 with a known duration of diabetes of less than five years, 40% of patients taking insulin and 24% of those not taking insulin are found to have retinopathy. 7,8 These numbers increase to almost 60% after 10 years and greater than 80% after 15 years. Approximately 25% of Type 1 patients have some retinopathy after five years. Using an Eidon True Color Confocal Scanner, this image shows moderate to severe NPDR with multiple cotton-wool spot and dot/blot hemorrhages. Two particular aspects of diabetes can put patients at risk for developing diabetic retinopathy: duration and glycemic control. This article explains the care diabetes patients require and details the biological processes that indicate where to classify a patient with diabetic retinopathy, as well as what treatment should follow. 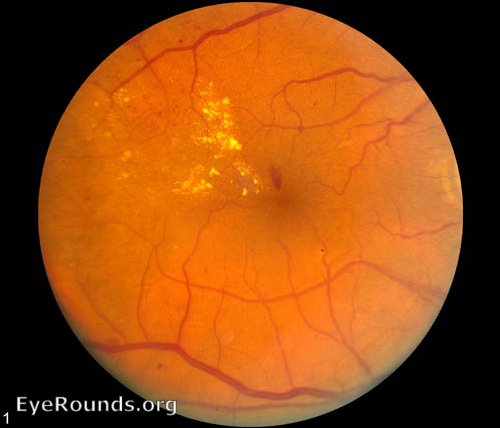
It may seem like minutiae, but even minor distinctions can be valuable as they inform our treatment protocol and, ultimately, prevent significant visual impairment for our patients. These categories are each further split by severity. In the case of diabetic retinopathy, these are divided, chiefly, into two: proliferative diabetic retinopathy and nonproliferative diabetic retinopathy. With management of this disease now firmly in optometry’s wheelhouse, the depth of research into its ocular impact has provided the ability to delineate its progression using various categories. Intraretinal hemorrhages similar to those found in the retinopathy associated to blood dyscrasias could be an association with SARS-CoV-2 in the context of a coagulopathy induced by the infection.ĬOVID-19 SARS-CoV-2 intraretinal hemorrhages novel coronavirus ophthlamology.To day, optometrists play a crucial role in managing diabetes, a leading-and growing-instigator of vision loss. After 1 month of the COVID-19 treatment, fundus examination improved and fluorescein angiography demonstrated no diabetic retinopathy signs, no retinal vasculitis and no significant delay in arterial or venous filling. Fundus examination revealed bilateral venous stasis and dot and blot intra-retinal hemorrhages preceding the diagnosis of COVID-19 in a patient with mild respiratory symptoms that progressed within a few days to a severe respiratory distress. We report here the first case of a patient with bilateral unusual dot-blot retinal hemorrhages and retinal venous dilation who presented shortly thereafter a PCR-proven COVID-19.Ī 59-year-old woman presented with a 7 days history of blurred vision in both eyes. As the pandemic is spreading and the whole picture is yet unknown, ophthalmologists should be aware of unusual ocular presentations of COVID-19 since they could precede the development of severe respiratory distress. There have been anecdotal reports of ocular manifestations in the Coronavirus Disease 2019 (COVID-19).
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
